Here are some interesting facts:
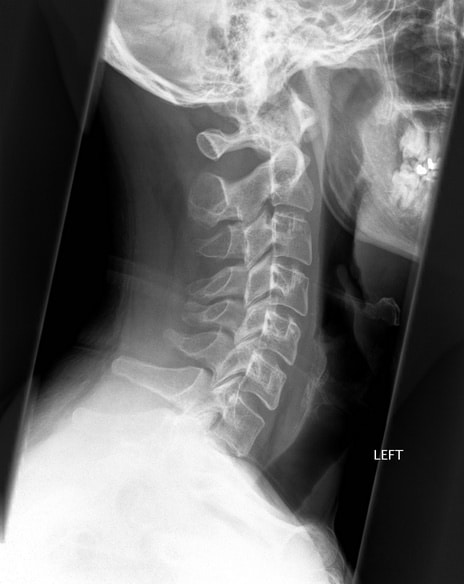
The Neck:
An MRI study of healthy adults and seniors found that 98% of all the men and women with no neck pain had evidence of “degenerative changes”in their neck. (1)
The Mid Back:
An MRI study of healthy adults with no history of upper or low back pain found that 47% had disc degeneration,53% had disc bulges and 58% had disc tears in their thoracic spine. (2)
The Low Back:
Lumbar disc degeneration is present in 40% of individuals under the age of 30 and present in over 90% of those between the ages of 50-55.(3)
The Knee:
Up to 85% of adults with no actual knee pain have x-rays that show knee arthritis. (4)
The Foot:
32% of people with no foot or heel pain have a heel spur visible on x-ray.(5)
The Shoulder:
MRI studies of adults who have no shoulder pain show that 20% have partial rotator cuff tears and 15% have full thickness tears. In addition, in those over the age of 60, 50% (half) of those who had no shoulder pain or injury had rotator cuff tears on their MRI that they did not even know about.(6)
Sooooo…….
Stop worrying about what your MRI and X-RAY may be showing, because scary findings do not have to equal pain and disability.
Start putting more effort into proactive management like physiotherapy and a healthy lifestyle to help deal with the acute pain of degenerative conditions so that it does not end up becoming a chronic condition.
If you’d like to discuss how we can help you to be proactive. Call and make an appointment today.
References:
1. Okada E, et al Disc degeneration of cervical spine on MRI in patients with lumbar disc herniation: comparison study with asymptomatic volunteers. Eur Spine J. 2011 Apr;20(4):585-91
2. Matsumoto M, et al Age-related changes of thoracic and cervical intervertebral discs in asymptomatic subjects. Spine (Phila Pa 1976). 2010 Jun 15;35(14):1359-64.
3. Cheung KM, et al Prevalence and pattern of lumbar magnetic resonance imaging changes in a population study of one thousand forty-three individuals. Spine (Phila Pa 1976). 2009 Apr 20;34(9):934-40.
4. Bedson J, Croft PR. The discordance between clinical and radiographic knee osteoarthritis: a systematic search and summary of the literature. BMC Musculoskelet Disord. 2008 Sep 2;9:116.
5. Johal KS, Milner SA. Plantar fasciitis and the calcaneal spur: Fact or fiction? Foot Ankle Surg. 2012 Mar;18(1):39-41.
6. Sher JS, et al Abnormal findings on magnetic resonance images of asymptomatic shoulders. J Bone Joint Surg Am. 1995 Jan;77(1):10-5.